You-Lin Qiao1†, Jose Jeronimo2, Fang-Hui Zhao1, Johannes Schweizer3, Wen Chen1, Melissa Valdez2, Peter Lu3, Xun Zhang1, Le-Ni Kang1, Pooja Bansil2, Proma Paul2, Charles Mahoney3, Marthe Berard-Bergery3, Ping Bai1, Roger Peck2,Jing Li1, Feng Chen1, injectable steroids for sale uk Mark H. Stoler4 and Philip E. Castle5
1Cancer Institute and Hospital, Chinese Academy of Medical Sciences and Peking Union Medical College, Beijing, People’s Republic of China
2PATH, 2201 Westlake Avenue, Suite 200, Seattle, WA
3Arbor Vita Corporation, 6611 Dumbarton Circle, Fremont, CA
4Department of Pathology, University of Virginia, Charlottesville, VA
5Global Cancer Initiative, 100 Radcliff Drive, Chestertown, MD
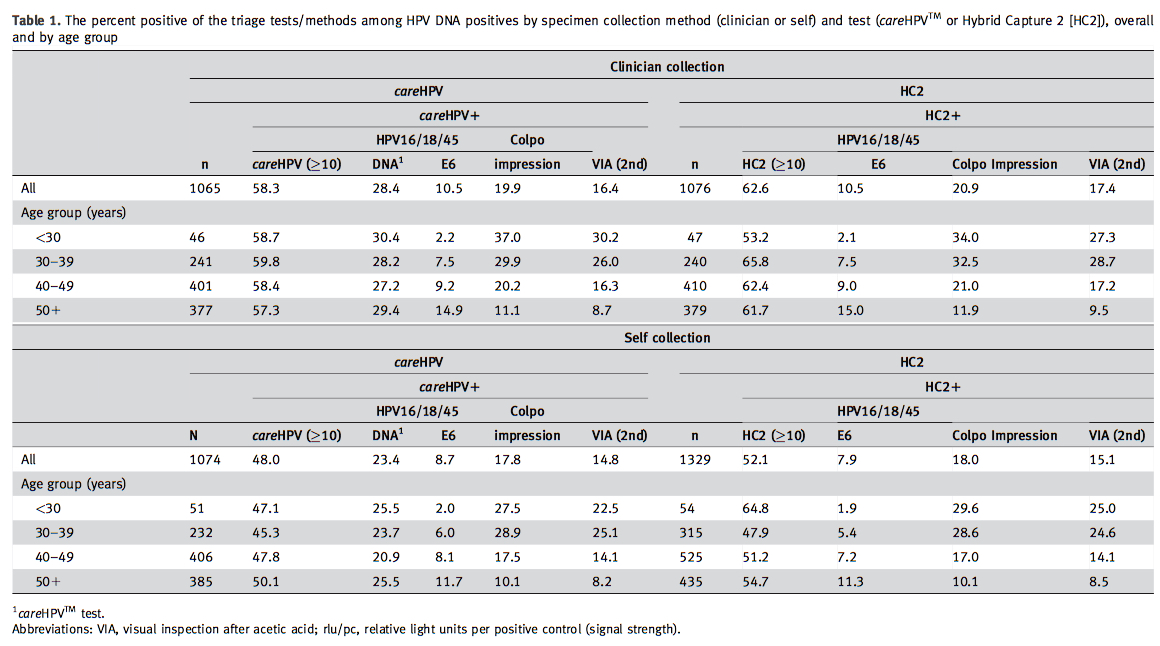
Using human papillomavirus (HPV) testing for cervical cancer screening in lower-resource settings (LRS) will result in a significant number of screen-positive women. This analysis compares different triage strategies for detecting cervical precancer and cancer among HPV-positive women in LRS. This was a population-based study of women aged 25–65 years living in China (n=57,541). Each woman provided a self-collected and two clinician-collected specimens. The self-collected and one clinician-collected specimen were tested by two HPV DNA tests—careHPV™ and Hybrid Capture 2; the other clinician-collected specimen was tested for HPV16/18/45 E6 protein. CareHPV™-positive specimens were tested for HPV16/18/45 DNA. HPV DNA-positive women underwent visual inspection with acetic acid (VIA) and then colposcopic evaluation with biopsies. The performance for detection of cervical intraepithelial neoplasia grade 3 or cancer (CIN31+) among HPV DNA-positive women was assessed for different triage strategies: HPV16/18/45 E6 or DNA detection, VIA, colposcopic impression, or higher signal strength (≥10 relative light units/positive control [rlu/pc]). The percent triage positive ranges were 14.8–17.4% for VIA, 17.8–20.9% for an abnormal colposcopic impression; 7.9–10.5% for HPV16/18/45 E6; 23.4–28.4% for HPV16/18/45 DNA; and 48.0–62.6% for higher signal strength (≥10 rlu/pc), depending on the HPV test/specimen combination. The positivity for all triage tests increased with severity of diagnosis. HPV16/18/45 DNA detection was approximately 70% sensitive and had positive predictive values (PPV) of approximately 25% for CIN31+. HPV16/18/45 E6 detection was approximately 50% sensitive with a PPV of nearly 50% for CIN31+. Different triage strategies for HPV DNA-positive women provide important tradeoffs in colposcopy or treatment referral percentages and sensitivity for prevalent CIN31+.
